PDF Handout
Graded Assertiveness
Many adverse outcomes in healthcare are a result of absent or incomplete communication. Strong verbal communication skills are key in coordinating teams and optimising the flow of information between colleagues.
Problems can arise for a number of reasons, but one common occurrence is failure of junior staff to question seniors about their actions. This can be especially problematic in the event of an acute patient deterioration such as the “Elaine Bromiley” case:
Short Video (2 mins):
The Full Video (13 minutes)
Having a specific concern about patient care is one thing, but bringing up the concern can often be a challenge. This is especially difficult when the concern is about a Senior’s actions. Sometimes, raising a concern can be very difficult because in an emergency situation time is limited and the clinical and personal consequences are uncertain for both parties and the process is seen as “counter cultural” in most healthcare systems.
Where your ‘boss’ is involved there may be many competing interests so raising a concern can feel like an impossible task.
This situation is (thankfully) rare but it is important to think about how you would broach the subject. Not having an approach could lead to patient harm.
Different Models of Communication
This brief video outlines the 4 commonly encountered communication styles in a hospital:
CLICK HERE
(1) Co-operative
(2) Assertive
(3) Submissive
(4) Aggressive
CUSS Model for Graded Assertive Communication
One suggested method of bringing to attention a potential error is Graded Assertiveness.
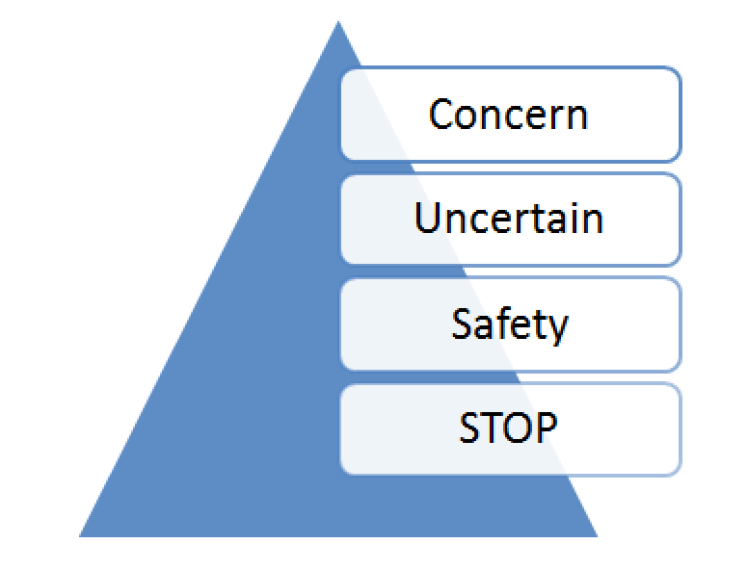
We suggest that you could gently “Cuss your Consultant”:
-
C – CONCERN – I’m concerned that allergies haven’t been recorded (we haven’t checked for allergies)
- U – UNSURE – I am uncertain if this Augmentin medicine can be given to someone with a possible penicillin allergy
- S – SAFETY – I am really worried it is UNSAFE to give this patient a penicillin like drug given his known allergy. I think this is a patient safety issue…
-
S – STOP – Please stop – we need to take a timeout and discuss this situation further or seek an alternative
PACE Model for Graded Assertive Communication
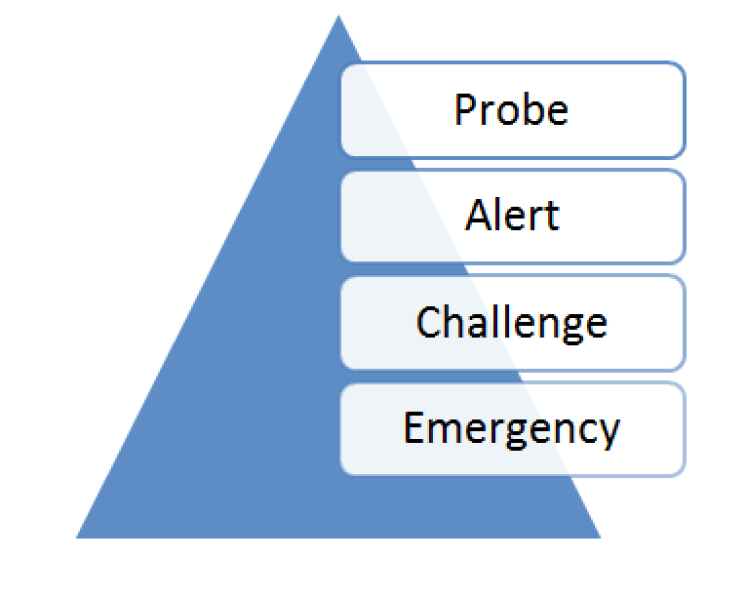
An alternative method, now endorsed by the Royal College of Anaesthetics in Australia and New Zealand is the SPACE Model:
This is derived from the “PACE” Model. In the same way as ‘CUSS’ the aim is a gradual rise in the firmness of the challenge. As a rule we should refer back to objective findings and observations about the patient rather than direct criticism of actions.
Final Thoughts
If you want to practice we suggest you try some simulation training or think about some scenarios. It might be worthwhile having a laminated version of the PACE or CUSS model on your badge for quick reference at the crucial moment.
As we become more senior it’s important to given our juniors permission to question us. We can teach them about Graded Assertiveness as well as consider our own potential responses to some of the key words outlined above. Thinking of my own clinical experience I believe Graded Assertiveness can be limited by the Senior clinicians variable response to the challenge.
In contrast, the airline industry has been forced to take on changes in communication based on a ‘challenge and response model’ to prevent future crashes. An example that comes to mind is the Tenerife Air Disaster in 1977:

The following excerpt is taken from the Journal of Air Transportation World Wide (1988):
Conclusions
In the same way as changes continue to be made in the aviation industry, we need to take action in healthcare to ensure the best possible outcomes for our patients and use of communication tools is just a small part.






Recent blog from ICN -http://intensiveblog.com/speak/