A Review of Venous and Arterial Blood Gases in Emergency Medicine
(POST UPDATED 20/3/21)
My recent ANZ General Medical Update Talk Slides:
You are a new staff member working in the Emergency Department (ED). During your induction you are introduced to the practical workings of the Point of Care Arterial Blood Gas (ABG) Machine in the ED:
As you struggle to listen to the machine company representative talking about ‘cleaning the machine’ you think about lunch and briefly recall that you fell asleep in all those boring basic science lectures…
Basic Sciences Recap
What basic science do you need to know to understand ABGs?
- pH
- pH is a measure of hydrogen ion concentration. In other words, a measure of the acidity or alkalinity of a solution. Aqueous solutions at room temperature with a pH less than 7.0 are acidic, while those with a pH greater than 7.0 are alkaline (basic).
- The Normal Physiological pH is around 7.4.
- Production of Acid in the Body:
- (1) Carbon Dioxide (CO2) – 15000 mmol/day
- Generates carbonic acid in combination with water
- (2) Non-volatile Acids – Up to 100 mEq
- Sulphuric acid derived from the metabolism amino acids
- Where does the Acid go?
- (1) Renally Excreted
- Kidney excretes acid by combing H+ with ammonium or phosphate based compounds
- (2) Respiratory Elimination
- (1) Renally Excreted
- (1) Carbon Dioxide (CO2) – 15000 mmol/day
- Production of Bicarbonate (Alkali) in the Body:
- This is mostly renal – often occurs as compensatory response to chronically high CO2
- The Primary Problem
- If pH < 7.35 primary problem is likely to be an acidaemia
- pH > 7.45 primary problem is likely to be an alkalaemia
- In other words, looking at the pH normally indicates the primary disorder:
- Acidosis/Acidaemia
- Respiratory – high CO2
- Metabolic – low HCO3 (bicarbonate)
- Alkalosis/Alkalaemia
- Respiratory – low CO2
- Metabolic – high HCO3 (bicarbonate)
- Acidosis/Acidaemia
- Base Excess
- This often confusing number on the ABG tells us how much alkaline (base) one would have to add in mmol/L to get to a neutral pH of 7.4. In other words a base excess of ‘MINUS 6’ means we would have to ADD 6mmol of bicarbonate to get to a pH of 7.4.
- Practically speaking the base excess (or base deficit) tells us whether there is a metabolic problem (regardless of the CO2 level that determines respiratory acidosis and alkalosis)
- The Henderson-Hasselbalch Equation
- Assessment of acid-base using the bicarbonate-carbon dioxide buffer system:
- Chemical Equation (equilibrium):
- CO2 + H2O <–> H2CO3 <–> HCO3- + H+
- As ‘carbonic acid’ in the body is negligible the following equation can be applied:
- pH = 6.10 + log ([HCO3] / [0.03 x PCO2])
- pH = 6.10 + log ([HCO3] / [0.03 x PCO2])
- ‘Conservation of Charge‘ – ‘ The Balance of Charges in the body:
- Positively Charged Ions such as Na+ (Cations) balance Negatively Charged Ions such as Cl- (Anions) – this happens as a ‘priority’
- Compensatory buffering with Bicarbonate (negative charge) or Protons (positive charge) occurs to compensate for imbalances in charge. This is known as a ‘dependent variable’
-
- So why is there an ‘Anion Gap’?
- Although these Charges always balance we calculate ‘Anion Gap’.
- Confused?
- The Anion Gap is the Gap between the MEASURED (not the total) Positive and Negative Ions
- What is the ‘Strong Ion Difference’?
- The ‘strong’ ions in the Body are Sodium (Na+) and Chloride (Cl-) and the Normal ‘gap’ between these should be about 38mmol/L. (e.g. Na 140 – Cl 102 = 38)
- Practically speaking if the Chloride goes up the Strong Ion Difference goes down and the body must compensate for the extra Anion (negatively charged chloride) with a positively charged ion. The freely available pool in the body of +ve charges is Protons (H+)! Therefore, when the chloride goes up we often see a Normal Anion Gap Metabolic Acidosis – the clinical significance of this may be limited outside the ICU setting, but its worth thinking about this when prescribing Fluids (e.g. Normal Saline, Hartmann’s and Plasmalyte).
Why Take a Blood Gas in the Emergency Department?
- Aids in diagnostics in many ED patients
- Helps guide management of sepsis, respiratory failure and cardiac arrest
- Point of Care testing is very fast and can speed up IV contrast imaging (Creatinine) and Electrolyte Correction (Na+, Ca++ and K+)
- Aids in ventilator management (Invasive and Non-invasive Ventilation)
Rules of the Blood Gas “Game”
- Don’t hurt the patient unnecessarily (first do no harm)
- Consider an Arterial Line (early in the ED stay) if the patient is really sick
- An arterial line in an appropriate patient is likely to save the patient (‘victim of venepuncture’) multiple painful needles in the ED and during their hospital stay…
- Consider doing a Venous Gas – much of the important blood gas information can be elicited from a venous blood gas (and it is much less painful)
- If you are going to do a blood gas don’t have multiple attempts in the same spot if you initially fail – either get someone else to try or consider trying the femoral artery, brachial artery or the other radial artery…
- Don’t take an unwell patient off their Oxygen to obtain the ABG Sample (i.e. any ED patient who needs a blood gas):
- This can precipitate rapid onset of life threatening rebound hypoxia
- Hypoxia kills in minutes – Hypercarbia kills in hours
- You can calculate the A-A gradient to figure out ‘relative’ hypoxia for patients on controlled Oxygen
- In Emergency Medicine a rise in CO2 is often due to fatigue and exhaustion (i.e. an Acute Problem)
- Don’t leave the blood gas unattended
- Get the sample to the lab (straight away on ice, and call the lab to let them know its coming)
- Alternatively, run the blood gas, preferably yourself, immediately after taking it…
- Interpret the ABG in the ‘clinical context’ of the patient in front of you
ABG Interpretation
- FIO2 – The percentage of inspired oxygen that you took the blood gas on
- pH (Normal Range 7.35 – 7.45)
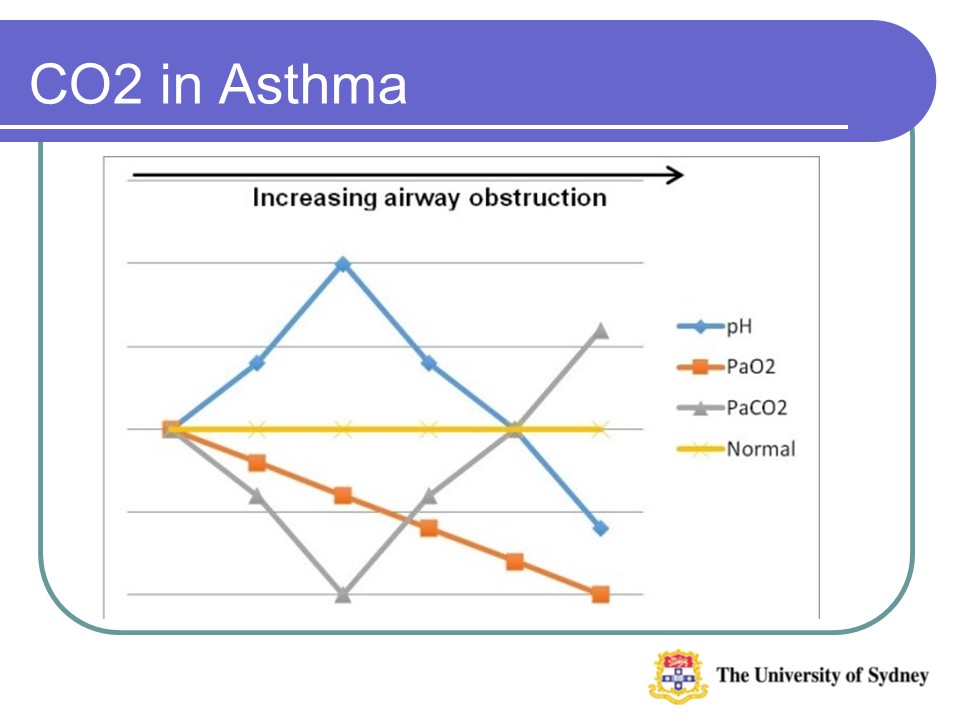
- PaCO2 – Partial Pressure of Carbon Dioxide (Normal Range 35-45 mmHg)
- PaO2 – Partial Pressure of Oxygen (Normal Range 80-100 mmHg on room air)
- HCO3 – Bicarbonate (Normal Range 22-28)
- O2% – Oxygen Saturations (Normal Range 95%-99%)
- B/E – The Base Excess (Normal Range -2 to +2)
- Others
- Electrolytes
- Lactate (correlates with mortality in sepsis)
- Renal Function
What is the Primary Problem?
- Identifying the primary problem is the first step in interpretation of the ABG.
- As mentioned above, the direction of the pH usually identifies the primary acid-base problem:
4 Important Steps
- Look at the pH – it indicates the type of primary disorder
- Note the PCO2 – tells us whether there is a primary respiratory problem
- Note the Base Excess – tells us whether there is an additional or primary metabolic problem
- Determine any compensation…
Is there any compensation for the primary disorder?
- Compensation can be Acute or Chronic
- Ask whether there is appropriate compensation for the primary disturbance?
- If there is a Respiratory Acidosis has there been any compensation?
- Is the Bicarbonate raised suggesting chronic respiratory hypoventilation (e.g. COPD)? As a general rule of thumb ‘compensation’ doesn’t correct the pH to baseline (i.e. a pH of 7.4)
- Is the Bicarbonate raised suggesting chronic respiratory hypoventilation (e.g. COPD)?
- If an acidosis is present calculate Winter’s Formula:
- Expected CO2 = 1.5 x HCo3 + 7
- Example:
- For a Bicarbonate of 10 – CO2 should =1.5×10+7 = 22
- If the CO2 is higher than this expected value this suggests inadequate respiratory compensation for the Metabolic Acidosis
- See below for ‘Advanced Compensations’
Metabolic Acidosis
The Anion Gap (A.I.G.)
- Calculated Anion Gap = Na – Chloride – HCO3
- The gap normally should be between 4 and 10)
- If the AIG is Raised this suggests the presence of a HAGMA
- The Causes of HAGMA are recalled by the mnemonic ‘CATMUDPILES’
- Finally, make corrections for the Albumin level if this is available:
- For every 10 below the Normal Albumin add 2.5 to the Anion Gap
- (*Normal Albumin is 40g/L so Albumin of 30 add 2.5 to AIG)
- Key Principle – Albumin is an anion and a weak acid
| HAGMA Table |
Classic Mnemonic – C.A.T.M.U.D.P.I.L.E.S. |
|
CO, Cyanide |
Alcoholic Ketoacidosis |
|
Toluene (abuse) |
Methanol, Metformin |
| Uraemia (Acute Kidney Injury, CRF) |
D.K.A. |
| Paraldehyde, Phenformin, Paracetamol, P.Glycol |
Isoniazid (INH), Iron |
|
Lactic Acidosis – Divided into Type A (imbalance between O2 supply and demand – tissue hypoxia) and Type B (no tissue hypoxia but instead a metabolic derangement) | |
|
Ethanol, Ethylene Glycol |
Sepsis, Salicylates (Aspirin) |

Is there an additional metabolic disorder?
- At this stage we may have several abnormalities on the blood gas
- To find ‘potential’ further problems some clinicians use a ‘Delta Gap’ calculation and other clinicians use Excess Gap Calculations:
- To Calculate the Excess Ion Gap
- Excess Gap = Anion Gap – Normal Anion Gap + Bicarbonate (HCO3)
- Here is an Example Case
- Bicarbonate = 16
- Case Calculated AIG = 14
- Normal AAG = 10
- Calculation for The Excess Gap = (14 – 10) + 10 = 20
- To Calculate the Excess Ion Gap
- The Excess Gap should be in the Range of the Normal Bicarbonate (24-28)
- If the Excess Gap is higher than this normal range for Bicarbonate (22-28), for example 30, then we can say that there is an additional problem in the form of a Metabolic Alkalosis.
- However, in this case the Excess Gap came to 20. If the Excess Gap Calculation comes to less than the normal range for Bicarbonate (22 – 28), then there is a third acid base disorder in the form of a Normal Anion Gap Metabolic Acidosis (NAGMA)
- Of course, NAGMA and Metabolic Alkalosis can be Stand-alone Disorders
- We need to know the causes of these disorders and remember to look for them even when we have found one metabolic problem already:
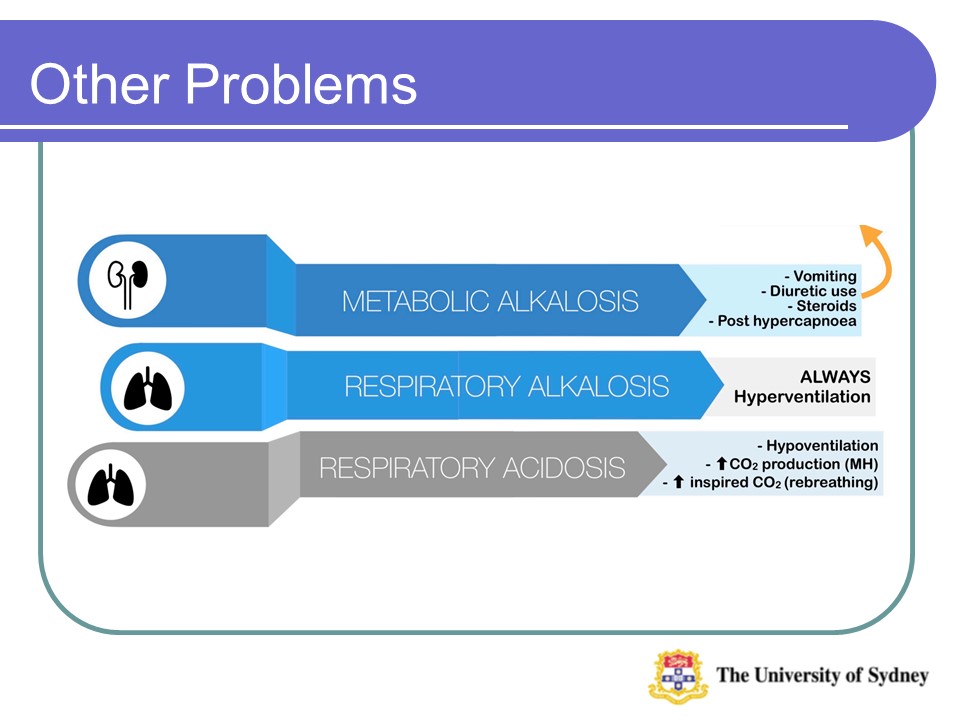
Causes of ‘NAGMA’ & ‘Metabolic Alkalosis’

The Venous Blood Gas
VBG v ABG
- We may be presented (increasingly) with Venous Blood Gases
- Differences are Subtle but important on Venous Gas:
- pO2 should be about 40mmHg (i.e. about the same as CO2)
- pH is about 0.05 lower on the Venous Gas compared with Arterial
- CO2 is about 6mmHg higher on the Venous Gas
- Bicarbonate is about 2 lower on the Venous Gas
- You might consider doing a Central Venous Gas (especially in Sepsis, where some ICUs doctors may get and ABG and Central Venous O2 to calculate fancy things like O2 Extraction. This is not relevant in ED). In the Rivers Study of Early Goal Directed Therapy in Sepsis they aimed for a Central Venous Oxygen Saturation CVO2 >70%
VBG Literature Review
(EMA 2010 Dec;22(6):493-7)
- Summary of the Review:
- The Mean arterio-venous difference in pH was 0.035 pH units (n= 1252), with narrow limits of agreement.
- The weighted mean arterio-venous difference for pCO(2) was 5.7 mmHg (n= 760), but with 95% limits of agreement up to the order of ±20 mmHg.
- For bicarbonate, the weighted mean difference between arterial and venous values was -1.41 mmol/L (n= 905), with 95% limits of agreement of the order of ±5 mmol/L.
- Regarding base excess, the mean arterio-venous difference is 0.089 mmol/L (n= 103).
- There is insufficient data to determine if these relationships persist in shocked patients
Summary
- In the vast majority of situations, as long as you can get a pulse oximeter on the finger, we don’t need an arterial blood gas in the ED. Obviously in many cases, the past literature (respiratory, ICU and surgical) is based on and therefore may mandate that you get an ABG.
- If the patient is shocked, correlation between VBG and ABG may not be accurate (as above). In these cases we may put in an Arterial Line and do serial Blood Gases.
- Serial VBGs may be a valid alternative to ABGs – for example in DKA cases
Advanced Corrections
- See above for a summary of basic calculated compensations
- Winter’s Formula is useful for the Expected CO2 but what about other compensations? What do we do when there is a Chronic High CO2 due to COPD – What is the expected Bicarbonate?
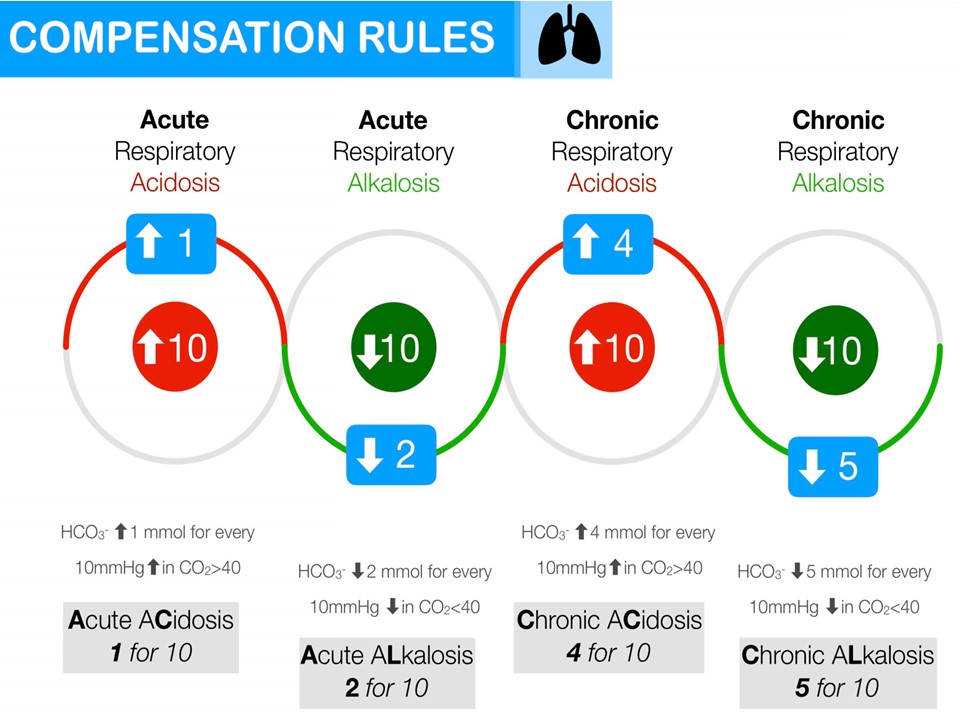
- For High CO2 – Chronic – Add 4 to the Bicarbonate for Every 10 rise in CO2 above 40mmHg
- For High CO2 – Acute – Add 1 to the Bicarbonate for Every 10 rise in CO2 above 40mmHg
- For Low CO2 – Chronic – Take 5 from the Bicarbonate for Every 10 decrease in CO2 below 40mmHg
- For Low CO2 – Acute – Take 2 from the Bicarbonate for Every 10 decrease in CO2 below 40mmHg
- Reverse Winter’s Calculation – For a Metabolic Alkalosis – for each rise in Bicarbonate above normal by 1 – Add 0.6 to the Expected CO2
Osmolality
- Osmolality of a solution is the number of osmoles of solute per kilogram of solvent
- Osmolarity of a solution is the number of osmoles of solute per litre of solution
- Osmolality is measured in mOsm/kg by laboratory machines called osmometers. Osmolarity is calculated from a formula which represents the solutes which under ordinary circumstances contribute nearly all of the osmolality of the sample
- Any gap between measured and calculated values may represent the presence an additional osmotically active substance – the causes of which are outlined in the table below…
Calculated Osmolality = 2 (Na + K) + Urea + Glucose + Alcohol
Alcohol is an important factor to consider
To Calculate Alcohol (Ethanol) Level there are various options.
If ethanol is reported in non-SI units, it is converted to mmol/L as follows:
- Ethanol mg/dL/4.6 or Ethanol % × 218:
- Alcohol of 45mg/dL = 0.045 % of alcohol
- 0.1 % = 22mmol (e.g. ‘1 %’ = 217mmol)
- Example: Ethanol 46mg/dl = (Ethanol/4.6 or x 0.218) = 10mmol of ETOH
- Estimating Levels fof Toxic Alcohol from the Osmolar Gap:
- Methanol – in mg/dl x (mmol) Osmo gap x 3.2
- Ethylene Glycol – in mg/dl x (mmol) Osmo gap x 6.2
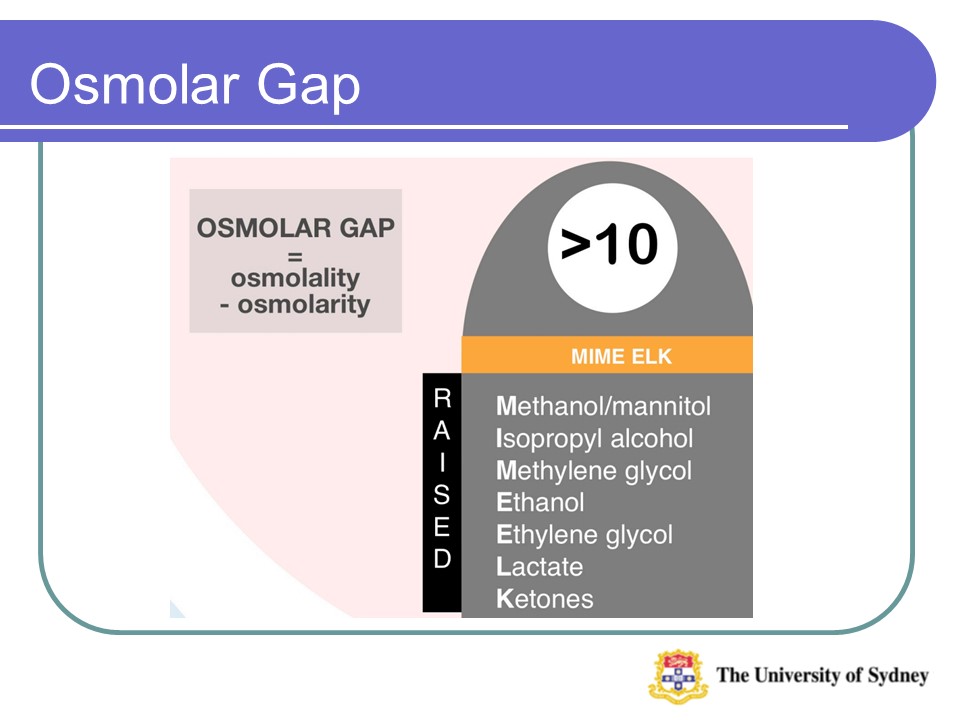
What are the causes of an increased osmolar gap?
Non Toxic Causes
Shock / Glycine / High Lipid and High Protein / Glycerol / Trauma and Burns
Toxic Causes
Ethanol / Sepsis / Methanol / DKA / Ethylene Glycol / Renal Failure / Propylene Glycol / Lactic Acidosis / Isopropyl Alcohol
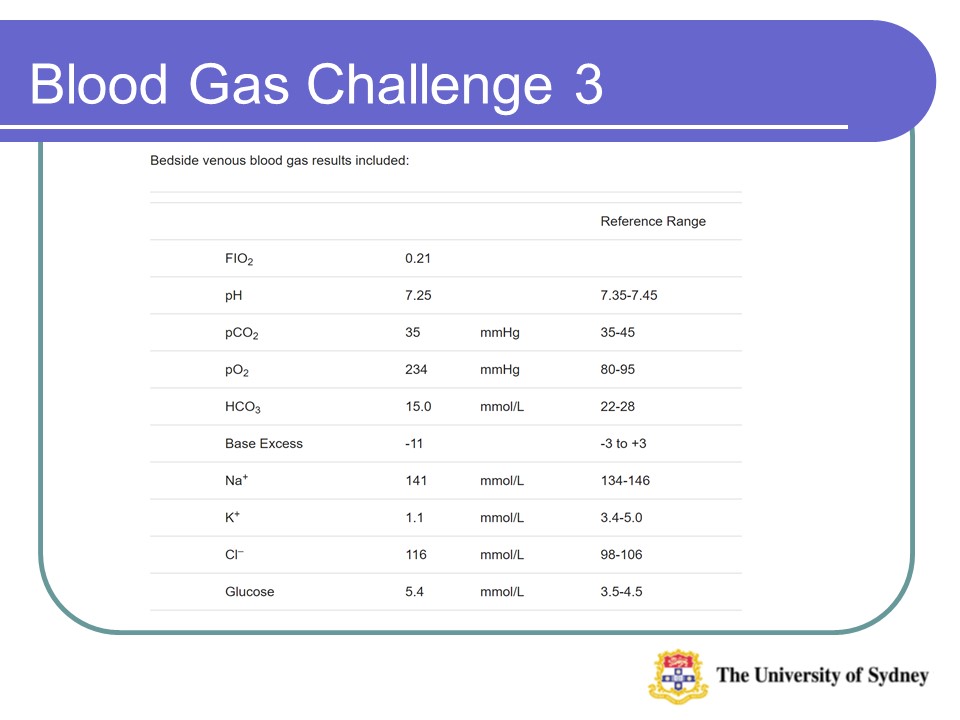
Blood Gas Cases
Further Reading and Links
- Printable Handout – Arterial Blood Gases Doc
- Venous Blood Gases – Venous Blood Gases
- Venous Blood Gases 2 – Venous Blood Gases
- Arterial Blood Gases (HABER) Practical Approach – ABG: Western Medical Journal PDF
- Arterial Blood Gases – EMCRIT – Blood Gases Part 1
- Arterial Blood Gases – EMCRIT – Blood Gases Part 2
- Arterial Blood Gases – EMCRIT – Blood Gases Part 3
- Arterial Blood Gases – EMCRIT – Acid Base Cheat Sheet – Acid Base Cheat Sheet – 2011
- Arterial Blood Gas – Overview Powerpoint – ABG Overview Presentation
- Severinghaus J W et al. Blood Gas Analysis and Critical Care Medicine. Am J Resp Crit Care Med (1998); 157: S114–22.
- EmergencyPedia CarCast – FACEM Metabolic
- Yale ABG Interpretation – Arterial Blood Gases
- ABG Overview – ABG Basics Overview PDF

Printable Handout – Arterial Blood Gases PDF
Blood Gas Worksheet (Checklist) – Download PDF