OVERVIEW
- There are 4 major ‘options’ to effectively manage the Airway in an Emergency.
- Everyday abilities at “1” and “2” are the most important competencies to have:
- Basic Airway Manoeuvres with use of Bag Valve Mask (BVM)
- A combination of option “1” with Adjuvant Devices such as oropharangeal and/or nasopharangeal devices
- Option 1 and 2 are the most important skills to practice diligently
- An invasive Supraglottic Airway (Laryngeal Mask Airway)
- Definitive Airway (either Endotracheal Intubation or access via the neck for an emergency subglottic airway)
BASIC AIRWAY SKILLS
- Assessment of Airway and Breathing
In order to assess airway and breathing: ‘DR-ABC’:
- Check for
- Danger
- Responsiveness of patient
- Open the airway with basic manoeuvres
- Remove obvious obstructions from the airway
- Listen, Look and Feel for Breathing
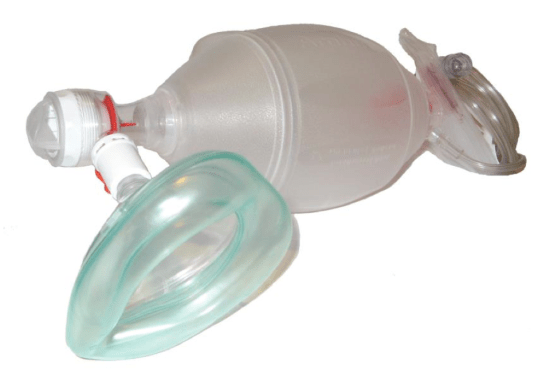
- Ventilation Devices – BVM
- Key Points to Successful Ventilation:
- Remember to connect the device to an Oxygen Supply
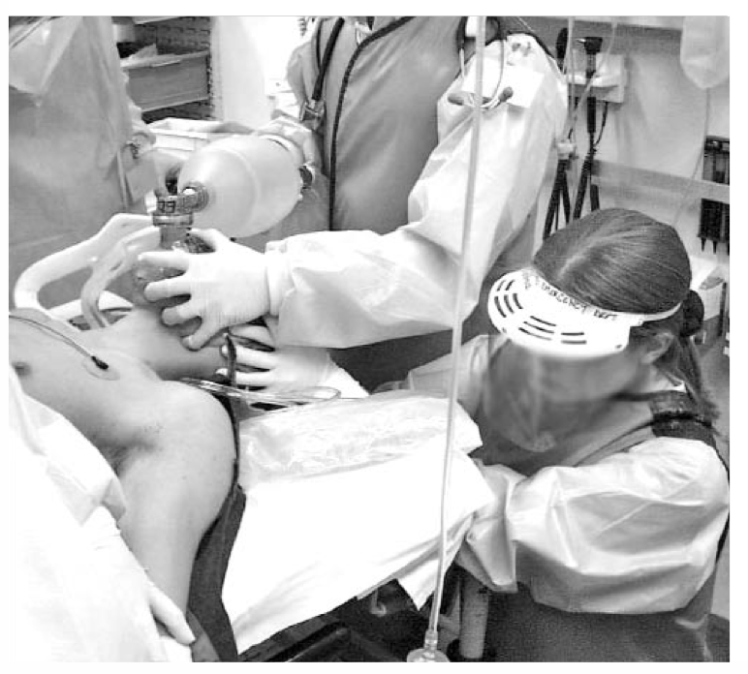
- Use two providers wherever possible (see External Study)
- Maintaining a good seal is important for ventilating the patient.
- This is done in basic terms by lifting the face into the mask and applying a steady downward counter pressure to the mask.
- Try placing your little, ring and middle fingers of your left hand on the mandible in the shape of the letter ‘M’ and your thumb and fore finger on the mask in the shape of a ‘C’.
- Now ask a colleague to squeeze the bag to Ventilate.
- Don’t ‘bag’ too fast or hard – we recommend aiming for 10-12 breathes / min
- average rate of ventilation can be >40 per minute in cardiac arrests (see External Study)
- If ventilation remains difficult consider an Adjuvant Device (see below)
- Patients receiving BVM for cardiac arrest can do as well if not better than those who are intubated (see External Study)
- Key Points to Successful Ventilation:
- Failure to Ventilate
- associated with ‘MOANS’:
- Mask Seal (Size, hands, shape, beard, trauma)
- Obesity/Obstruction (Resistance, shape, faster desaturation)
- Age (Over 55 and pregnant women are harder)
- No Teeth (Face ‘falls’ inward)
- Stiff Lungs (Asthma, COPD etc)
- associated with ‘MOANS’:
UPPER SUPRAGLOTTIC DEVICES
- Commonly used adjuvant devices include the OROPHARYNGEAL and NASOPHARYGEAL airways:
- In the case of difficult ventilation in a patient who is not breathing or in the unconscious patient who is still breathing these devices may help you maintain the airway:
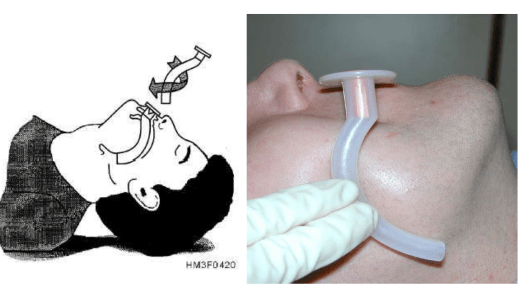
- The Nasopharyngeal Airway
- Apply Lubricant and consider placing a pin through airway
- Place through nostril with a slight twisting motion straight back into nasopharynx
- Attempt to ventilate Patient with bag mask
- Avoid use in head injuries, facial injuries and with epistaxis
- The Oropharyngeal Airway
- For adults size the airway from the tragus of the ear to the edge of mouth
- Insert upside down and rotate backwards over the tongue
- In children place the device in the ‘right way round’ to avoid trauma to the upper oropharynx
LOWER “SUPRAGLOTTIC” DEVICES
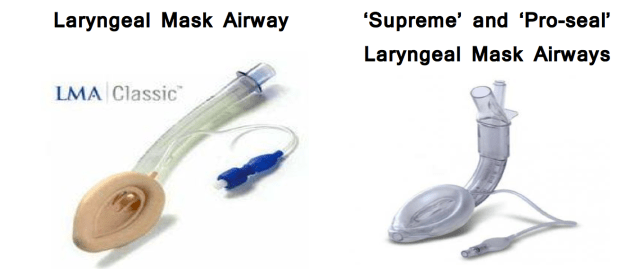
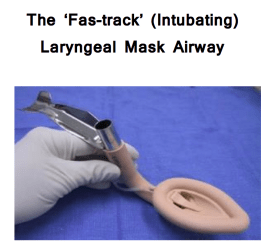
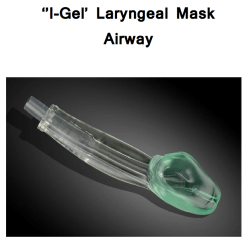
The Laryngeal Mask Airway (LMA)
Dr Archie Brain developed the Laryngeal Mask Airway in the UK during the 1990s. Its widespread introduction has revolutionised Anaesthetics. These devices can be used for many day case type procedures and are also very useful in the Management of the Emergency Airway especially where attempts at Intubation have failed. They are increasingly recommended in the management of Cardiac Arrests. These airways are sometimes called ‘Supraglottic Devices’
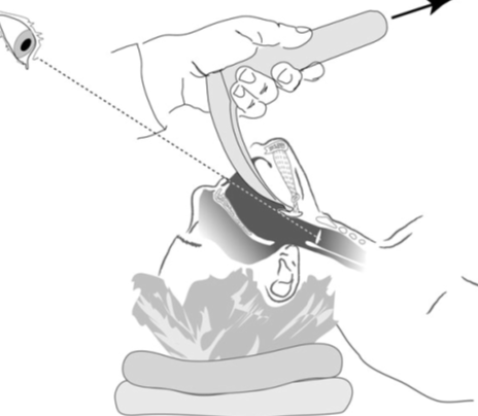
For the Laryngeal Mask Airway the insertion technique is similar to placing an Oropharyngeal Airway. Slide device with steady pressure into the mouth towards the floor then round the back of the tongue with pressure towards your hips. You may feel a distinctive ‘pop’.
LMA Insertion Demonstration – CLICK HERE
After successful insertion remember to inflate the device before attempting to ventilate (you often see and feel a ‘pop)’. Some advanced devices have a port for a Nasogastric tube.
ENDOTRACHEAL INTUBATION
A systematic assessment of the patient’s airway is important prior to attempting intubation. Bear in mind that many ‘difficult‘ airways are not predicted often despite an airway assessment. Regardless, an attempt to anticipate how difficult an airway intervention is advised.
Of note, in the mid 2020s it has now become usual practice to use Video Laryncoscopy routinely and often learn this technique first. It is advisable to learn both direct and video techniques if you can though the learning curve is faster for video…
In order to assess the ‘potential difficulty’ of intubation – we can use the ‘LEMON’ law:
- Look
- Evaluate ‘332’
- Malampatti Score
- Obstruction
- Neck
Intubation (Key Points may apply to both DIRECT and VIDEO)
- Prepare your Equipment in Advance of Procedure
- You will need appropriately sized endotracheal tubes, suction (working), equipment for ventilation (bag mask), pillow or head ring for head position, adjuvant equipment such as introducers and alternative blades to hand.
- Head position – Does the tragus of the ear line up with the sternal notch?
- Check the Laryngoscope is working (is the light on?)
- Hold handle in Left Hand (right hand is free to move the head and hold the tube)
- Place the Laryngoscope blade into the Right side of the mouth with help of an assistant if necessary
- Sweep the Tongue across to the left in order to push it out of the way…
- Insert the blade until you Visualise the Epiglottis

- Lift the Laryngoscope Handle forward with steady force (do not ‘lever’ teeth)
- Look to Visualise the Vocal Cords
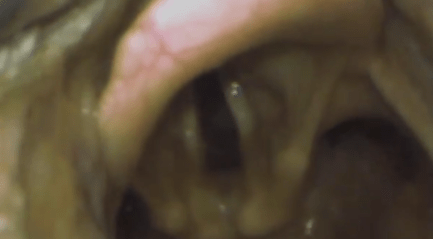
- Optimise your view if necessary using “30 second drills“

- Place the tube or ‘boogie‘ introducer through the cords (and ensure to visualise it going through).
- Be careful not to put ET tube in too far (if you do you may go past the carina and only ventilate the right lung)
- Connect the Bag and Valve Mask, Ventilate the Patient Gently and then Inflate the Cuff until any leaks disappear
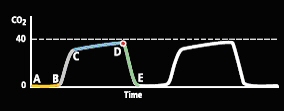
- Connect the End Tidal CO2 (trace and tubing pictured below)
- Check the air entry on both sides in 3 positions to ensure equal air entry and then Secure the ET tube with tape or tie
- Document in the patient’s medical record

Equipment
Various equipment must be prepared prior to advanced airway management.
The commonly used laryngoscope ‘blades’ include the MACINTOSH, MCCOY and MILLER types:

Other Methods
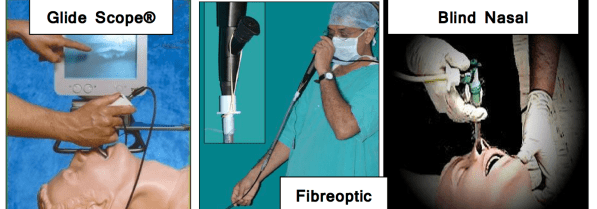
Other complex techniques are used selectively by airway specialists (anaesthetists) for securing an airway. These may include ‘awake’ intubation by ‘blind nasal’ route or ‘fibreoptic’ method. This is often facilitated by the use of sedation and local anaesthesia.
Since about a decade ago developments in technology have increased the availability of devices such as the “C-mac” and “Glide Scope” (VIDEO LARYNGOSCOPY). These provide excellent views on an electronic viewing screen and are relatively easy to learn quickly.
Rapid Sequence Intubation (RSI)
“Rapid sequence induction (RSI) is the standard procedure for prompt induction of anaesthesia and subsequent intubation used in the Emergency Department and ICU as well as in selected cases in the Operating Theatre.”
CLICK HERE for more information about RSI
A CHECKLIST is recommended when carrying out this complex and challenging team based procedure
EMERGENCY SURGICAL AIRWAY
Surgical Method
Pros – Higher Success in NAP4 Study
Cons – Bleeding, Fear
Needle Method
Pros – Most clinicians have familiarity with basic skills needed, Less Fear
Cons – Failure in NAP4 Study, Temporising only
Jet Insufflation
- Jet Insufflation can be used to oxygenate the patient where bag mask ventilation becomes impossible or inadequate.
- Jet Insufflation for oxygenation can be achieved simply by using a needle cricothyroidotomy (see video above) in order to achieve rescue oxygenation a simple cannula placed in the trachea is connected to the wall oxygen supply
- Assemble a simple circuit using:
- 3 way tap for connection to cannula
- 5 ml syringe with the bung removed attached to the 3 way tap
- Simple oxygen tubing inserted into the back of the syringe
- As an alternative you can use a pre-assembled circuit (some are specially designed for this purpose)
- The circuit needs to have a hole which when occluded allows controlled flow of gas into the patient.
- You can use a 3 way tap or cut a hole in the oxygen tubing.
- The thumb is used to occlude the hole intermittently typically with a ratio of 1:4 (higher ratios may be safer)
- The Jet airway method can only be used for a short period
- Why?
- CO2 will accumulate due to no gases being able to come out of the lungs (in other words this method can oxygenate but not effectively ventilate the patient)
- Why?
- The Jet Insufflation method may buy some extra time while a definitive airway can be established. It is especially useful in children because an open surgical procedure is very difficult in children under 10 due to size of the trachea
Quick Pre-workshop video:
FURTHER ‘FOAM’ LINKS
- Sydney HEMS Intubation Workshop – CLICK HERE
- BVM Ventilation Overview – CLICK HERE
- Overventilation is Common – CLICK HERE
- BVM versus Intubation in Cardiac Arrest – CLICK HERE
- Jet Insufflation and Needle Cricothyroidotomy – CLICK HERE
- Needle Cricothyroidotomy – CLICK HERE
- Can’t Intubate Can’t Oxygenate (CICO) APLS – CLICK HERE
- Potential Jet Ventilation Dangers – CLICK HERE
- PDF handout – AIRWAY WORKSHOP




Thanks Andrew. This looks very clear and understandable. Sadly, my browser removes any pictures but the writing looks good!
I’ve been mentally sifting through our long case patients – I think you have most of them from past years – but you’re welcome to have a look at the summaries we made for them and see if there are any that would fit the bill.
Amanda
_________________________________________________________________
Dr Amanda Harrison MB.BS, MPM, MMedEd
Senior Lecturer, Medical Education
Sydney Medical School – Westmead | Faculty of Medicine
THE UNIVERSITY OF SYDNEY
C24 Westmead Hospital | Westmead NSW | 2145
T +61 2 9845 6403 | F +61 2 9891 3749 | M +61 412 081 528
E amanda.harrison@sydney.edu.au | http://sydney.edu.au