The ECG Page
[Download a Printable Handout of this Page – ECG Handout]
Thanks for visiting the EmergencyPedia page. Since we started in April 2013 we’ve been keen to include an ECG page to share our ECG collection.
In combination with textbooks and real life ‘on the floor’ cases, we think that the web is a great place to go for the up to date Electrocardiography education…
ECG interpretation is a core skill for emergency doctors, nurses and paramedics! There are already lots of high quality dedicated ECG (EKG) ‘FOAM‘ websites that we would recommend:
Emergency Medicine Top links
Introduction
Why is ECG interpretation an important clinical skill?
On a daily basis nurses, paramedics, cardiologists, GPs, physicians and many other practitioners routinely record and interpret ECGs. In the acute care setting a busy workload means that it can be challenging to accurately interpret all these tests in a short time. Core theoretical knowledge and practice of interpretation allow the learner to develop skills in ECG pattern recognition…
Furthermore, EmergencyPedia notes that in the Australasian Emergency Fellowship Examination ECGs constitute 25% of the Visual Aid Question (VAQ) component.
ECG interpretation is likely to remain a high yield topic in the future in many medical, nursing and paramedic exams. This is all for good reason, as the ECG is a commonly performed test in Acute Medicine and it is often poorly interpreted especially when a systematic approach is not applied.
The use of a Systems and Checklists
We have developed a systematic approach of interpreting ECGs that can be used as a learning tool or as a checklist. Learning this type of approach will probably be useful for both for ECG clinical cases and for passing exams (such as the FACEM Fellowship). In both these situations (e.g. real life or an examination) ECGs need to be accurately interpreted under significant time pressure.
Our experience was that gradual study of an ECG textbook combined with using a systematic approach to ECGs encountered at the hospital quickly build up both theoretical knowledge about the ECG as well as an ability to recognise common problems…
If you are new to ECG interpretation, using a methodical approach at first helps develop the pattern recognition abilities that are common in expereinced doctors and nurses… (i.e. a good example of pattern recognition in clinical practice would be a nurse’s “endofthebedogram” or “gestalt“ suggesting that the patient is in hypovolaemic shock – she knew this was likely to be the problem because she had seen it many times before in her career).
There are lots of examples of checklists in medicine (e.g. Intensive Care, Theatre and Intubation) and the experienced clinician can also make use of checklists and templates.
It is often said that the most commonly missed injury is said to be the “second injury”. This second injury or problem often goes unnoticed due to a sense of ‘relief’ or ‘satisfaction’ which comes from the practitioner discovering the first abnormality… Human errors (that we are all at risk of making) are common and often predictable. Some of the common error producing pitfalls have been described as ‘Search Satisfaction’, ‘Confirmation Bias’, ‘Anchoring’ and ‘Premature Closure’. These pitfalls are summarised in the following link and picture:
Dr Chris Nickson’s Cognitive Pitfalls
How is all this relevant to ECG interpretation? We believe that the same error producing pitfalls described above are also possible in the interpretation of ECGs. Jumping to a dignosis without a checklist or systematic approach could be perilous as significant pathology could be missed.
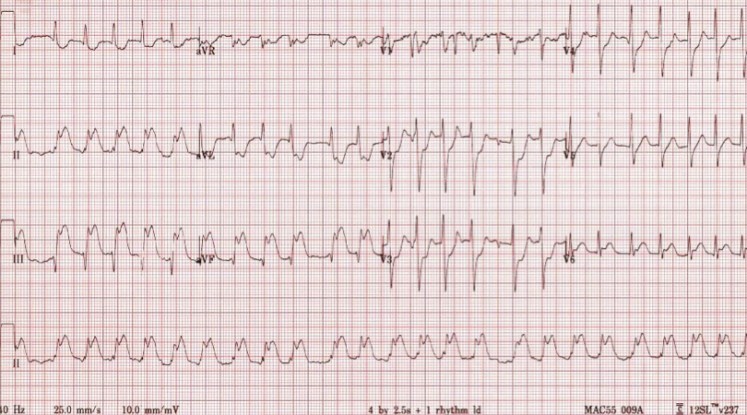
You might notice that on the following ECG case example that the patient is in ‘Rapid Atrial Fibrillation’ just by a cursory glance. However, it would be easy to miss the ‘Inferior Myocardial Infarction’ if you were distracted by the first (most obvious) abnormality…
The ECG Checklist
An ECG checklist or template, not only serves as a good learning tool for the novice ECG reader, but also should be useful for more experienced clinicians who are aware of ‘human factors’ and don’t want to miss significant abnormalities on the ECG.
ECG Basics – Recording the ECG
- This is a common OSCE STATION in Medical Student Exams
- Start with washing your hands and making sure the ECG machine is clean…
- Take the ECG machine to the bedside (plug in as necessary)
- Introduce yourself to the patient
- Check the patients name and I.D. wrist band
- Ensure privacy
- Ask for a chaperone to assist you as appropriate
- Explain to the patient what the ECG involves and what it is looking for
- Generally we need informed consent:
- “This is a routine test looking at the electrical activity of the heart. To do the test we need 3-5 minutes of your time. We will place about 10 sticky labels n your legs, arms and chest and connect some wires to the sticky labels. The machine then detects the activity of the heart. The machine doesn’t give you a shock and the test (shouldn’t be painful). The requesting doctor will look at your ECG test once it has been printed on the paper… Do you have any questions or concerns about having this test done?”
- Generally we need informed consent:
- Input patient details into the ECG machine
- Place the ECG Dots on the chest, legs and arms
- Arms (AVR (right) and AVL (left))
- Legs (AVF)
- Chest Leads
- V1 at 4th Intercostal Place at right sternal border
- V4 mid clavicular line at the 5th intercostal space
- V6 mid axillary line at the level of V4
- Record the ECG (i.e. press the record button)
- Print and label the ECG
- Indicate if there was any chest pain when the ECG was taken
- Thank the patient, clean the machine’s leads and wash your hands
Does every patient need an ECG?
- Not every patient needs an ECG. However, the ECG is a cheap and reproducible test which is a standard investigation in the work up of many undifferentiated presentations in the Emergency Department (ED).
- Most advocate the liberal use of ECGs for Chest Pain patients but it is also useful in most medical and toxicological patients in the ED.
- An early review of any ECG taken is important because conditions readily diagnosed on the ECG such as Acute Myocardial Infarction are time dependent emergencies that are ideally recognised and treated as soon as possible. Therefore, viewing of ECGs by a senior doctor early is mandatory in many Emergency Departments.
- More about the efficient and safe work-up of chest pain patients can be found in the following NSW health document published in 2011 – Chest Pain Quality Improvement
ECG Basics – An Interpretation System
We found the process of learning ECGs frustrating at times. Despite many books and apps reassuringly titled along the lines of ‘the ECGs made Easy‘ there is, in fact, often a significant degree of difficulty when starting learning about ECGs.
Rest assured, time and patience will get you to your goals eventually…
We suggest you practice as many ECGs as you can both from books and on the wards.
Dr Ken Grauer’s ‘Pocket Brain’ resource is an up to date adjunct for learning at the bedside.
Find a copy by Clicking Here.
The EmergencyPedia ECG System
- Identify Demographics (name of patient, time take, old ECG for comparison)
- Identify as a Complete 12 lead ECG (e.g. not a derived ECG from a monitoring system)
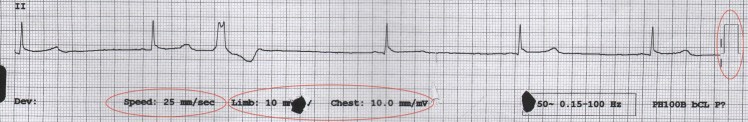
- Check Paper speed (25mm/s)
- Standard Calibration is 5mm by 10mm
- On the ECG look at the bottom centre (paper speed) and bottom right (calibration ‘vertical block’ of 10mm) for these details
We have circled the key areas to check in the following ECG portion:
- At a paper speed of 25mm/s:
- A ‘BIG’ square is 0.2 seconds in duration and a ‘SMALL’ square is 0.04 seconds
Click Here for more on ECG Basics
- RATE, RHYTHM and AXIS
- Rate (Big Squares are 0.2 seconds at a paper speed of 25mm/s) = 300/R-R interval squares
- Rhythm (Card Method)
- Axis
- Lies at 90 degrees to Isoelectric Lead
- This AXIS is Normal if I and II have a positive deflection and AVR is negative
- Define the Baseline
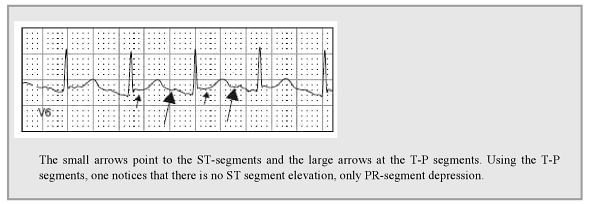
- Look at the ‘TP’ Segment – use this to define ‘ST segment elevation’ and ‘PR depression’
- The importance of this is described by Brady and Mattu in the following figure:
- Look at the ‘TP’ Segment – use this to define ‘ST segment elevation’ and ‘PR depression’
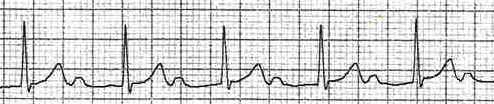
- P waves
- P waves correlate with Atrial electrical activity arising in the Sino-atrial (SA) Node
- The P wave is marked with the Red Arrow:

- Ask yourself:
- Does each QRS complex have an associated P wave?
- Is the rhythm Nodal in origin (Narrow Complex, No P Waves) or Ventricular in origin (wide complex and No P wave)
- Types of P wave:
A Bifid P wave – May suggest Left Atrial Enlargement
Peaked P wave = P-pulmonale – This can represent Right Atrial Hypertrophy or represent ‘a pseudo peak’ (Hypokalaemia)

Absent P Waves – Think of AF (most common), sinoatrial blocks, junctional and ventricular rhythms
- PR interval
- What is the PR interval?
- It should be 0.12 to 0.2 seconds
- It is measured from the start of the P wave to the start of the QRS complex
- Is the interval constant?
- Is there a QRS complex for every P wave?
- What is the PR interval?
Specific PR Interval Problems
Is there a 1st degree heart block? (See ECG 14 below)
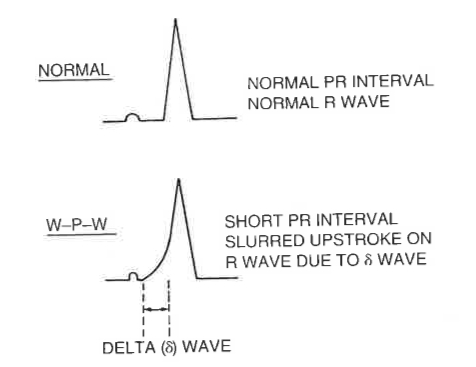
Wolf-Parkinson- White Syndrome (WPW) type I is Upright Delta Wave in V1
WPW type II is Down-going Delta Wave in V1
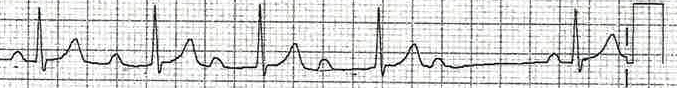
If increasing PR interval – Consider Wenkebach’s Phenomenon (AKA Mobitz I) – See ECG 13
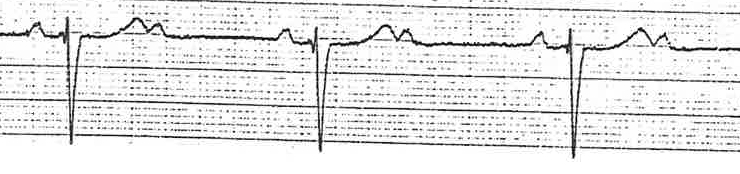
If constant but a QRS is dropped regularly – Consider Mobitz Type 2 Heart Block
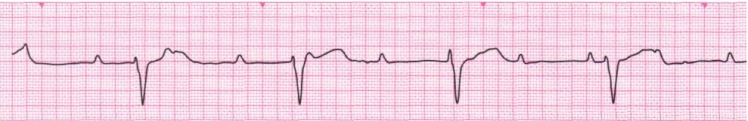
P waves seen but NO association – this may be 3rd degree (complete) Heart Block
- PR Segments
- Depression in most leads or elevation of the PR segment in AVR is suggestive of Pericarditis when associated with concave up ST elevations globally
- Q waves
- Non pathological waves are common
- These represent normal L-R depolarization in the septum
- Pathological is likely with the following:
- Non pathological waves are common
– Q waves more than 40ms (1mm) wide
– Q waves more than 25% of R wave or Q waves more than 2mm deep
- QRS Complex
- The QRS Complex (marked with the Red Arrow) should be less than 0.12 seconds or 3 small boxes

- When prolonged suggests a conduction delay as depolarization occurs across the Myocardium (There is the bundle of His which becomes a right bundle, a left bundle with 2 fascicles (anterior and posterior) – these can become ‘blocked’ as a result of conduction delay due to Myocardial Ischaemia, Drugs or Electrolyte Abnormalities
- Look at the Chest leads V1 – V6
- If shaped as an ‘M’ in V1 (that is mostly positive RSR pattern in lead V1) and ‘W’ in lead V6 think MARROW – Right Bundle Branch Block
- If shaped as W in V1 and M in V6 thing WILLIAM – Left Bundle Branch Block
- You can have Unifascicular Block (that is an isolated BBB), Bifascicular Block (classically RBBB with Left Axis Deviation) and Trifasicular (RBBB, LAD, Heart block)
- ST segments (depression or elevation)
- Elevation or depression of the ST segments classically represents Ischaemic Heart Disease and/or Myocardial Ischaemia. The elevation or depression is measured from the J point
- J Point (the junction of the QRS complex and beginning of the ST segment)
- How much is too much? This depends on the lead – in the Chest lead 2mm of elevation in 2 leads if significant, in the limb leads (further away) 1mm is significant
- QT interval
- Represents Potassium channels – i.e. a marker of repolarisation
- Drugs or disease that cause QT interval prolongation can lead to sudden syncope or sudden death due to an arrhythmia called Torsades de Pointes (Twisting around the point). This is also known as Polymorphic Ventricular Tachycardia.
- While rare QT prolongation is a concern. Treatment includes Magnesium and Potassium infusions.
- Consider using the QT nomogram to estimate risk of Torsades:
- Represents Potassium channels – i.e. a marker of repolarisation
- T waves
- If peaked think about Hyperkalaemia. If Inverted (outside of III and AVR) think about Paediatrics (T wave inversions are normal in Kids) and young females (also normal variant). Pathological Causes of T wave inversion include Myocardiac Ischaemia, Pulmonary Embolism, Cardiomyopathy, Electrolytes Disturbances and Stroke (especially Haemorrhagic)
- U waves (and T-U fusion)
- Can be seen when the K is low – an ‘extra’ wave ‘blip’ after the T wave
- J waves (Osborn)
- When seen are suggestive of Hypothermia
- An Epsilon Wave
- Rare finding that suggests Arrythmogenic Right Ventricular Dysplasia (potential for sudden death)
- Check for Pacemaker
- Various problems and presence of a pacemaker are detected on the ECG
ECG interpretation is about pattern recognition. However, so as not to miss subtle abnormalities, and to gradually build up to an adequate level of expertise we need to practice.
In doing this it is best to use a systematic approach such as the approach outlined above. The best way to learn is to go through lots of sample ECGs (the textbooks below are good resources for this) and take a problem based approach to learning the theory…
We recommend various websites and books (not paid by them) including the following:
ECG Cases
ECG Blogs
DR SMITH’S – ECGs (Minnesota, USA)
KEN GRAUER – ECGs (Florida, USA)
AMAL MATTU – ECGs (Baltimore, Maryland)
ECG WAVE MAVEN (Harvard, Massachusetts)
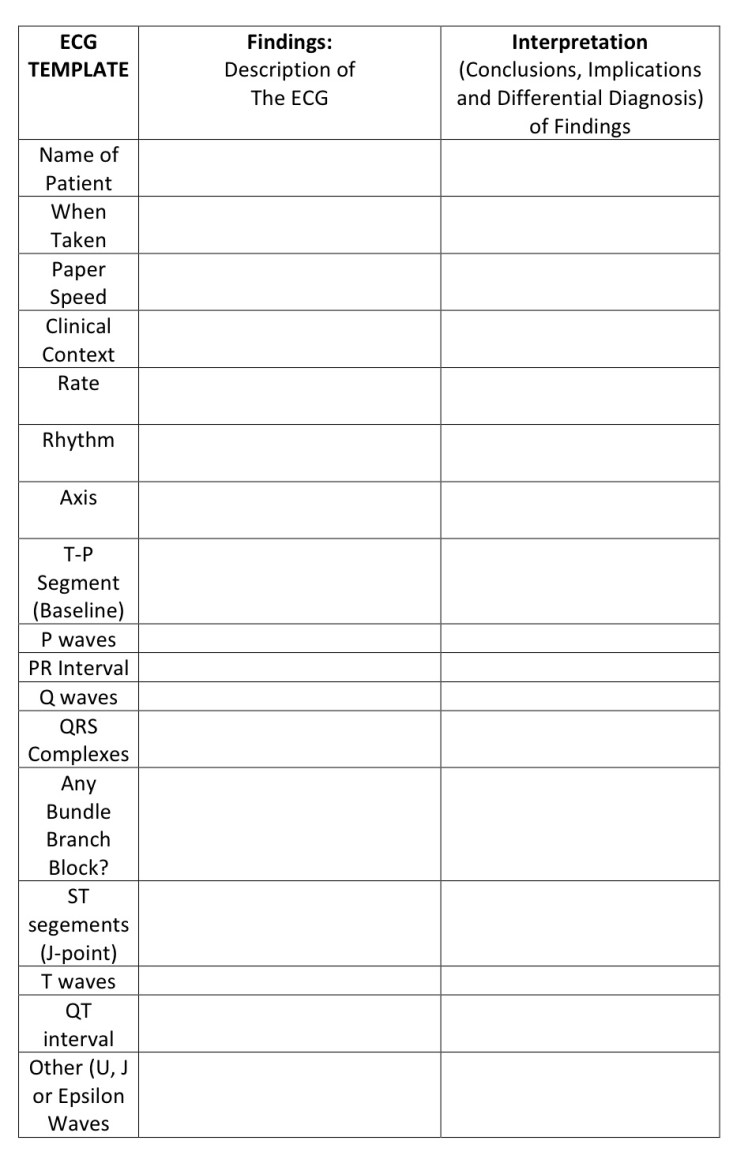














MUTH THANKS
Very good ECGs and explanations.
ECG 16:
Is it wellens or the patient is having a STEMI?
patient is still symptomatic,ST elevation and raised troponin.
Wellen’s : patient asymptomatic, and negative biomarkers…
thanks
Thanks. I guess it’s NSTEMI with Wellen’s ECG so you are right. Classic Wellen’s will be biomarker negative and often asymptomatic at presentation (chest pain resolution) then have a near LAD occlusion at angio… Can’t remember the exact story but for the purposes of ethics I’ve changed all the stories to “case vignettes”
LITFL AXIS review – http://lifeinthefastlane.com/axis-bold-love/
Wellen’s case and other cases have moved to https://emergencypedia.com/ecg-cases/
“Thank you for sharing this informative post about 12-lead ECG. As a medical professional, I appreciate how detailed and comprehensive your explanation is, making it easy for both novice and experienced practitioners to understand. It’s amazing how much information we can gather from a simple test like an ECG, and how crucial it is in diagnosing various heart conditions. Keep up the good work in providing valuable resources for the medical community!” Visit: https://www.tricog.com