The Internship of 2015-2016
Introduction
Changes in the Life of an Intern
Life as an Intern was pretty simple in the past. As recently as 2005 a typical internship in the British Isles and other Commonwealth countries consisted of 6 months of medicine and 6 months of surgery.
You’d be working for a ‘firm‘ – part of the same team for 6 months… You would also be expected to work a horrendous number of on-call shifts, sometimes 24 hours on call with minimal recovery.
This sentiment is graphically and somewhat cynically dramatised in the controversial 1990s BBC television show ‘Cardiac Arrest’ (worth watching a few episodes if you have time):
To comply with patient safety concerns as well as the European Union’s Working Time Directive and other legislation, the working system for Junior Doctors has been changed to keep interns away from most after hours duties (e.g. night shifts). There has also a movement towards a shift pattern type of working week with either 8, 10, 12 or 14 hour shifts.
The changes in the working hours of Junior Doctors in most developed countries has the advantage of limiting burnout and maximising educational and day time training opportunities. There are also perceived service provision benefits when out of hours ward cover is provided by more experienced practitioners. Unfortunately the disadvantage of changing working hours is a relative lack of exposure to emergencies and overall experience in the first year of working as a doctor. Some of this lack of exposure may be offset by Training in Simulation but it cannot be ignored as a potential issue.
The Intern of 2013 can expect to work around 75-90 hours a fortnight depending on local regulations. In the UK an Intern will do 4 different 3 month jobs in their first year whereas in Australia Interns usually do 5 terms lasting 10 weeks in their internship. With increasing numbers of graduates there are also multiple supernumerary jobs. Interestingly, United States Interns are still expected to work much longer hours that those described above.
Old Training System Features (A Historical Picture)
- Living on Site and a focus on Social Activities
- After-hours On-call
- Working Weeks of over 50 hours/week
- Working on a single ward and with the same people for up to 6 months
- Nights incorporated into every term
- e.g. one week of nights every 8 weeks on rolling roster
- No paid overtime
- Less Supervision
- Non-specific Curriculum for Junior Doctors
- Subjective Workplace Assessments (WPA)
New Training System Features (The Future)
- Assessment and Appraisal
- May include 360 degree feedback (Multi-source Feedback)
- Teaching and Education for Adult Learners
- High Level of Competition for Training Jobs (this is not new but is increasing)
- Working Weeks of 40 hours/week or less
- Mix of during hours and after hours
- Use of alternative training methods (the end of “see one do one teach one”)
- Objective Workplace Assessments (WPA)
- Managing Emergencies less on your own –If you do encounter an Emergency due to “MET Call” Systems are early detection of the deteriorating patient the Intern or Resident is likely to be in secretarial or minor medical role.
- Age at graduation is higher – issues with work-life balance
- Less after hours cover (when not doing a relief term)
- Less pay (due to less working hours)
- More stress due to various factors including time pressures and government targets
Tips for the New Junior Doctor
Safe Prescribing
It is essential to think about a safer approach to prescribing.
Recognition that this is a high risk activity in the day of the Junior Doctor is important.
- Problems with Prescribing should be anticipated (Murphy’s Law)
- Mistakes happen – and you are especially at risk if you are:
- (1) Inexperienced
- (2) Interrupted
- Try to avoid interruptions when you are writing drug charts by not attempting to multi-task when writing a drug chart. Only allow interruptions for true emergencies.
- (3) Have Limited Time for each task
Of course all of these factors apply to most interns…
- Resources for Safe Prescribing are available in book as well as rapidly searchable electronic format for your Smart Phone and Computes (click on the links below):
- Common areas that are associated with problems:
- Antibiotics – given to patients with an allergy (e.g. Augmentin and Timentin to Penicillin Allergic Patients)
- Antibiotics where levels are used for monitoringWarfarin
- Gentamicin
- Vancomycin
- Analgesia
- Treat the patient’s pain as a priority
- Use appropriate doses of opiates (e.g. 0.1mg/kg of Morphine for Acute Pain) and take advice from Pain Services or Palliative Care where needed
- Use the WHO Analgesic Step Ladder
- Dose Reduce Paracetamol where appropriate
- Warfarin
- Methadone and Buprenorphine
- Sleeping Tablets (including Benzodiazepines)
- Elderly PatientsUse a Protective PPI for patients on potent drugs like Steroids, Aspirin and NSAIDs
- Avoid BAN – benzodiazepines, anti-cholinergics, NSAIDs if possible
- Dose reduce renally cleared medications such as Digoxin
- Follow Up of the Ward
- Once your Drug Chart is written it is a legal document and it will be used for up to 7 days
- Where resources allow a pharmacist can review your medication chart on request – this can be useful for patient safety and for education
- Using Brand Names can lead to transcribing errors when the chart is rewritten or the patient is discharged – a classic case of this occurred in Australia – Colgout (Colchicine) was miscopied as Progout (Allopurinol) – the patient was on Azothioprine – this lead to a predictable drug interaction due to the reduced metabolism of Azothioprine. This is turn caused Neurtropenic Sepsis and an unfortunate fatal outcome. This drug interaction is well described in the literature.
- Avoid using Brand Names to avoid the above risks and to save the hospital pharmacy money
- How do we get Information about the patient’s medicines?
- Pharmacy Prepared Drug Packs (e.g. Webster Packs) – generally reliable
- The Handbag: ‘medication list’ (may be incomplete or out of date)
- Nursing Homes List (may be incomplete or out of date)
- Be Aware of the High risk of Non-English Speaking patients (they are at higher risk of harm from drug errors)
- The reliability of the Drug history varies from case to case
EmergencyPedia’s ‘Golden Rules’ for Prescribing
- If someone questions an order always double-check what you have written…
- Be nice to nurses and pharmacists – if they say your wrong you are probably wrong
- Always Check Dose if Unsure (MIMS, AMH)
- Never Prescribe brand Names if not familiar with the drug
- Always Re-Check Chart and PRNs, Always Write in BLOCK CAPS and Never write in Red or Green or Blue
- Always Repeat Uncharted Order Back in the Resus Bay.
- Write Drugs mixed in Fluids on the Fluid chart (Heparin) – use your local protocols
- Take a Break!
Summary
- Follow the ‘Golden Rules’ of Prescribing
- Don’t Use Brand Names
- Always Check the MIMS, AMH or similar standardised drug information resource
- Use your Phone, IPAD or Computer to make checks quickly
Managing People
Managing your interactions with colleagues, patients and relatives are all part of personal and professional development. Quality of relationships in the workplace makes a big difference to your job satisfaction as well as your effectiveness as a practitioner.
Communicating with Patients
Always think about asking the patient the following things:
- What is you major concern right now?
- What are you most worried about? (you may be surprised at the answer)
- Is there something else?
- Is there anything I can do to make you more comfortable?
- “I’m going to be looking after you during your stay in the Emergency Department – if there’s anything you are very worried about or unsure of don’t hesitate to ask for me.“
Try to Elicit “ICE” – this is the patients Ideas, Concerns and Expectations
Take a detailed Social History
Communicating with Consultants
Talking to consultants can be the most stressful part of being a Junior Doctor. Confusingly, what is expected in Medical Assessments such as OSCEs and Long Case Exams is different from the recommended way of talking to colleagues. Handover and discussion of patients were labelled as areas of concern in The Garling Report. As a result, standardised methods of communication such as “ISBAR” or “ISOBAR” are often recommend as a tool for communicating with other medical staff.

General Tips for Dealing with Consultants
-
Prepare your information and resources before you call
- Anticipate information you’ll need for the call (e.g. results)
- Consultation when you Need Something or have a Specific Clinical Question
- Be nice (kill them with kindness)
- Don’t respond in a passive or rude manner (even if the consultant you are calling is coming across as rude – you may have interrupted their dinner and they are a human being so give them the benefit of the doubt).
- Listen Carefully to advice from the Specialist
- This involves you being brief with your explanation
- Use The I S B A R Framework (see above)
- Don’t talk for too long – it’s not a long case presentation…
- Negotiate (see below)
- Show Respect for the colleagues opinion – show respect for their point of view even if you don’t agree with them…
- Compromise
- Be specific about your concerns and questions
- It may take a few calls to get what you need
- “If I send that D-dimer off straight away are you happy to have a look at the patient for me? I think they’d benefit from you having a look.”
- Close the loop – repeat back what has been discussed – cross-check what will happen with the patient
- When you ask for a consult or review of a patient you are “breaking bad news“
Medical Negotiation Skills
“Credibility, authority, and being LIKED are powerful persuasion tools” Cliff Reid (2013)
Negotiation Strategies
See also our review of Team Training – Click Here
- Authority
- Individuals are more likely to comply with experts/authority – you may not have this as an intern but your may be able to call on the help of someone who has…
- Reciprocity (“Do us a favour”)
- If you give something to people, they feel compelled to return the favour.
- e.g. “It sounds like the d-dimer sounds like an important test for you to have – I’ll make sure that gets done right now if you wouldn’t mind seeing the patient in the next 20 mins or so?”
- If you give something to people, they feel compelled to return the favour.
- Scarcity
- This is less applicable to medicine – i.e. rare items are more valuable to people
- LikingCommitment
- We are more inclined to follow the lead of someone who is similar to us rather than someone who is dissimilar
- Consistency
- Social Proof
- We view a behaviour as more likely to be correct if others are performing in a similar manner.
Managing Emergencies
The key issues with dealing with medical crises in the hospital is to anticipate and plan your behaviour and actions. Learning from each emergency you attend is also important and the best way to do this is to debrief immediately after (hot debrief) and with reflection some time later (cold debrief). Keeping yourself relatively calm and doing the basics well should be your focus when managing a cardiac arrest.
The infamous novel ‘House of God‘ says:
The following video produced by our simulation lab shows many of the key principles of managing an Emergency:
Another useful resources is the Crisis Code Course which gives practical tips on managing Emergencies from an American Emergency Medicine perspective.
Essential Crisis Management Skills
The Concept of Human Factors
Know about the Concept of ‘Human Factors’
We suggest you think about management of the TEAM, YOURSELF and the ENVIRONMENT in order to remain in control when managing difficult situations:
- YOU – Are you H.A.L.T?
- Hungry, Angry, Late or Tired – ‘stop yourself’ making a mistake if you are
- ENVIRONMENT – Are you familiar? Noise Levels (patient, team)? Distractions?
- Use Checklists to control the Emergency and free up your brain to think clearly
The highly functioning TEAM requires good leadership and followership to move forward effectively and efficiently towards shared common goals. As the team leader it is important to continuously allow for feedback, share your thought processes and summarise at regular intervals. As a team member it is important to provide feedback and support for the team dynamics to work well…
Elements of Good Teamwork
- A Clear Team Structure
- Adequate plan and preparation
- Skilled Members – (recognition of extra needs is part of good team work – call for help early)
- Effective Team Leadership
- Good Team Communication
- Full utilization of resources
- Wise management of people
- Share Common Goals
- Collaboration
- Regular Education and Training
When managing an Emergency Share your goals with the team (rather than a list of tasks).
Communicate using names and closed loop communication.
Debrief after Difficult cases and Emergencies and reflect on what went well and what could go better.
Try to share your thoughts and learning points with seniors as well as Interdisciplinary Team Members e.g. Nurses).
You should never feel completely isolated at a big hospital – there’s support available.
Graded Assertiveness
Raising a concern about a Senior’s actions in an Emergency can be very difficult and can feel like an impossible task. One suggested method of bringing to attention a potential error is Graded Assertiveness – we suggest you gently “Cuss your Consultant”:
- C – CONCERN – I am concerned that we haven’t checked for allergies
- U – UNSURE – I am uncertain that this Augmentin duo forte medicine can be given to someone with a possible penicillin allergy
- S – SAFETY – I am really worried it is UNSAFE to give this patient a penicillin like drug given his known allergy. I think this is a patient safety issue…
- S – STOP – Please stop – we need to take a timeout and discuss this further…
Recent Issues in the Medical Training System
The year in the life of an intern in 2013-2014 has changed a lot compared to twenty years ago when many of our hospital specialists and GPs graduated from Medical School. The first year as a doctor has even changed significantly compared to 5 years ago when most registrars and trainees became interns.
The large number of graduating medical students has increased the number of interns significantly. This pattern has occurred in Australia as well as many other developed countries. A full list of statistics for Australia can be found if you Click Here.
As a result of problems with similar transitions in the UK system some Australian authors predicted there may be problems with increasing number of students and that early planning would need to occur to avoid the problems seen in the UK.
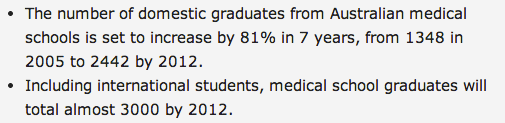
Increasing the number of graduating medical students should theoretically (at least in the government’s eyes) meet the demand for doctors both in urban and rural settings. However, the financial and logistical costs of training the increasing number of interns is very high. This has lead to a shortfall of places for the increased number of medical students to work and this in turn has lead to a great deal of stress for supervisors and applicants.
Some have labelled this mismatch as a crisis – and it certainly mirrors my memory of the UK system between 2005 and 2007 where there were similar stresses for medical students and junior doctors.

The Effects of changes in Training
Having noted some of the current issues with the training system that have recently taken place, it is highly likely, as was the case in my own experience of the UK system that ‘things tend to work out‘ for the individual. Even though the process is competitive, we have not tended to see the majority of medical students or junior doctors left out of desirable and fulfilling jobs in their training. Having said this, we do see and experience a lot of stress in getting to these goals. In some cases the stress of the application process has lead to doctors in training filing legal action due the perception of unfairness in the system. As long as the system is fair and has a degree of transparency hopefully we won’t see the same problems here in Australia over the next 5 years.
Finding your Career Path
Medicine holds an amazing number of “careers within a career” fitting a range of interests and lifestyle choices. Our main tip in choosing a career is to take advice from multiple sources including both trainees in that speciality and more importantly consultants in your chosen field of practise who are less likely to be burned out and more likely to reflect your long term career. You are likely to spend more time as a consultant than a trainee even if you change between specialties a few times or start late. We suggest inviting doctors in your area of interest to talk about themselves and their career. Most human beings won’t say no to this type of invitation. It’s simply a quick meeting where you ask them about their career and why they chose it – most people like to talk about themselves to some degree so don’t be scared to ask questions about why the consultant chose their career.
If you are not sure about what you want to specialise in you should be reassured that this is common – we advice you look at multiple options and take into account where you want to be in 10 years time in terms of both career and your home life.
Jesse Spur from Injectable Orange blog and podcast has an excellent 10 minutes spiel about being a great intern (well worth a listen) – CLICK HERE
Conclusions
In conclusion, being a new intern is one of the most exciting times of your life in medicine and while it required both stamina and patience it is a truly rewarding experience. Furthermore, the Junior Doctor has the opportunity to spend time with and learn from patients at the coal face of healthcare. The learning curve is steep in the first year as a doctor but the leaps forward that are taken in a short time are always apparent. The future holds ongoing and new challenges for the aspiring intern but none of these are insurmountable to the enthusiastic new doctor.
Good luck with your first year as a Doctor!!






2 thoughts on “Tips for The Junior Doctor of 2015”
Comments are closed.